Cervical Cancer Awareness: What You Need to Know About Cervical Cancer
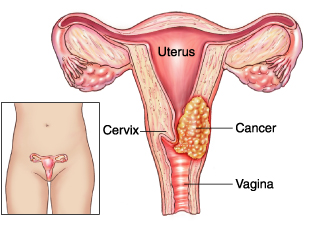
What is Cervical Cancer?
Cervical cancer is a condition that arises when normal cells in the cervix—the lower part of the uterus that connects to the vagina—accumulate abnormal changes in their genetic material (DNA mutations) and transform into harmful cancer cells. The cancer cells grow uncontrollably, live longer than usual and invade nearby cervical tissues. In advanced stages, the cells can spread to nearby lymph nodes and distant organs, such as the lungs, liver, and bones, through a process known as metastasis.
Cervical cancer is the fourth most common cancer among women worldwide, with approximately 662,000 new cases and around 349,000 deaths attributed to the disease in 2022.
The number of cases is higher in low- and middle-income countries, where there is limited access to human papillomavirus (HPV) vaccinations, screenings, and treatment options.
Such limitations often lead to in late-stage diagnosis and poor disease outcome for affected women.
Why Do People Develop Cervical Cancer?
Cervical cancer develops over several years, usually from pre-cancerous changes in the cervical cells.
It arises primarily from persistent infection with high-risk types of human papillomavirus (HPV), a common sexually transmitted virus, combined with other genetic and lifestyle-related factors.
Risk factors for cervical cancer include:
- Human Papilloma Virus (HPV) Infection: HPV infection is found in almost all cases of cervical cancer. The high-risk types of the virus, HPV 16 and HPV 18, are responsible for around 70% of cervical cancers globally. HPV causes precancerous changes in cervical cells, which if not detected and treated, progress to invasive cervical cancer over 10 to 20 years.
- Cigarette smoking: Cigarette smoking is an environmental factor that influences the risk of cervical cancer. The link between smoking and cervical cancer has been proposed to be likely due to the accumulation of chemicals in cervical mucus leading to DNA damage, decreased immunity and higher rates of genital HPV infection in smokers.
- Prolonged usage of oral contraceptives: Some studies found that prolonged use of oral contraceptives for more than five years increases the risk of cervical cancer among women who have HPV infection.
- Many full-term pregnancies (high parity): Women who have more than four full-term pregnancies have a higher risk of cervical cancer than those with fewer full-term pregnancies and those who have never given birth. The decline in parity in association with other factors might have contributed to a decrease in cervical cancer incidence in some countries.
- Early onset of sexual activity and multiple sexual partners: These factors increase the risk of infection with HPV and the likelihood of cervical cancer.
- Decreased immunity: People who have HIV infection and other immunodeficiency conditions have a higher risk of cervical cancer because their immune systems are not strong enough to fight HPV infection.
- Lack of screening and limited healthcare access: Screening can detect HPV infection and abnormal cervical cells early before the onset of cancer. Inadequate screening in low- and middle-income countries has been associated with a late-stage diagnosis of invasive cervical cancer.
- Genetic factor: Some people are prone to cervical cancer because they possess an abnormal gene.
How is Cervical Cancer Diagnosed?
Cervical cancer diagnosis involves some steps:
- Cervical screening: includes Pap smear and HPV test. Pap smear (cytology) is a screening procedure in which a sample of cells is taken from the cervix to detect abnormal changes early before they develop into cancer.
HPV Test: looks for high-risk HPV infection capable of causing abnormal changes in the cervix that have the potential to form cancer. - Colposcopy: This is done when abnormal cervical changes or high-risk HPV are detected during screening. During colposcopy, a magnifying instrument called a colposcope is used to examine the cervix. Prior to examination, the cervix is stained with specialised liquids: acetic acid, which stains abnormal areas of the cervix or Lugol’s iodine, which highlights healthy areas of the cervix. A small tissue sample (biopsy) may be taken from suspicious areas of the cervix for processing in the laboratory and microscopic examination (histology) by a pathologist to detect cancerous changes.
- Biopsy: small tissue samples taken from the suspicious area of the cervix are examined under a microscope by histopathologists for definitive diagnosis. Types of cervical biopsy include:
Punch biopsy – small samples are taken from the surface of the cervix.
Cone biopsy – a cone-shaped piece of tissue is removed from the cervix. It may be both diagnostic and therapeutic (curative) in early disease stages. - Imaging and Staging: imaging tests are used to assess the disease stage (how far the cancer has spread) after cervical cancer is confirmed. Examples of the imaging techniques are:
- MRI scan of the pelvis
- CT scan of the chest and abdomen
- PET-CT in selected cases
The FIGO (International Federation of Gynaecology and Obstetrics) staging system and TNM system describe whether the cancer is confined to the cervix or has spread to surrounding tissues, lymph nodes or distant organs.
What Are the Types of Cervical Cancer?
Cervical cancers are classified according to the type of cell they start from and their microscopic (histological) appearance. Types of cancers include:
- Squamous cell carcinoma (SCC): begins in the thin, flat squamous cells that cover the outer surface of the cervix (also known as the ectocervix). It is the commonest type, accounting for about 80–85%of cervical cancers globally.
- Adenocarcinoma: adenocarcinoma arises from glandular cells lining the inner canal of the cervix (also known as the endocervix). It accounts for around 10–25% of cases of cervical cancer. (References)
- Adenosquamous carcinoma: contains both squamous and glandular components.
- Other rarer tumours include small cell neuroendocrine carcinoma, clear cell carcinoma, etc.
What Are the Symptoms and Signs of Cervical Cancer?
Cervical cancer may cause no symptoms in early stages, hence the need for regular screening. As the disease progresses, you may experience:
- Abnormal vaginal bleeding: It is the most common symptom of cervical cancer and could present in the following ways:
- Intermenstrual bleeding (bleeding between periods)
- Post-coital bleeding (bleeding after sexual intercourse)
- Post-menopausal bleeding (vaginal bleeding after menopause)
- Abnormal vaginal discharge: Watery, bloody, or foul-smelling discharge
- Pelvic pain: could present as
- Persistent lower abdominal or pelvic pain or
- Pain or discomfort during sexual intercourse (dyspareunia)
- Symptoms of advanced stages: include unexplained weight loss, fatigue, lower back pain, leg swelling, or difficulty passing urine or blood in the urine if the tumour presses on or invades the bladder.
Many other conditions (such as fibroids, infection, or hormonal changes) can cause these symptoms. However, any persistent abnormal bleeding or discharge, especially after sex or after menopause, should prompt urgent review by a healthcare professional.
How Can Cervical Cancer Be Prevented?
Cervical cancer is preventable through a combination of vaccinations, screenings and healthy lifestyle choices.
- HPV vaccination: The HPV vaccine protects against the high-risk HPV types that cause the majority of cervical cancers, as well as some cancers of the vulva, vagina, anus, penis, and head and neck. WHO recommends HPV vaccination for girls aged 9–14 years, using one or two doses depending on national policy. It’s expected that 90% of girls should be fully vaccinated with the HPV vaccine by the age of 15. In the UK, the HPV vaccine is recommended for all children aged 9 to 13 years and people at higher risk from HPV.
- Regular cervical screening: Cervical screening detects HPV and cell changes long before cancer develops, allowing early treatment and prevention. In the UK, women aged 25–64 are invited for screening, generally every 5 years if they test negative for high-risk HPV. Those who have HPV infection are tested more regularly.
- Safer sexual practices: use of condoms, limiting sexual partners and avoiding very early onset of sexual activity reduce the chance of exposure to high-risk HPV.
- Smoking cessation: quitting smoking reduces the risk of cervical cancer and improves the body’s immunity against HPV infection.
- Improved Body Immunity: maintaining a healthy immune system through diet and exercise also aids in clearing infections.
What Treatment Options Are Available for Cervical Cancer?
The choice of treatment depends on:
- The stage of the disease
- The type and size of the tumour
- The need to preserve fertility
- The person’s overall health
Management is usually planned by a multidisciplinary team comprising gynaecological oncologists, clinical oncologists, radiologists, pathologists, specialist nurses and other professionals.
The treatment options for cervical cancer include:
- Surgery: This is often the main treatment for pre-cancerous changes and cancer confined to the cervix.
- Large Loop excision of the Transformation Zone – abnormal tissue is removed using a heated wire loop
- Cryotherapy or thermal ablation – freezing or destroying abnormal tissue
- Cone biopsy – removal of a cone-shaped piece of cervical tissue. It is done for small, localized lesions
- Trachelectomy – removal of most of the cervix while preserving the uterus. It is done for in young women who desire future pregnancy.
- Hysterectomy – involves the removal of the uterus and cervix, sometimes along with the lymph nodes.
- Radiotherapy: uses high-energy radiation to kill cancer cells. It is often combined with chemotherapy (chemoradiation) for locally advanced disease. It may also be used after surgery if there is a higher risk of recurrence.
- Chemotherapy: uses anti-cancer drugs that circulate in the bloodstream to kill cancer cells. It may be used before surgery (neoadjuvant) or after surgery (adjuvant), or on its own for advanced/metastatic disease to shrink tumours and relieve symptoms. Commonly used medicines include cisplatin, carboplatin, paclitaxel, and others in various combinations.
- Targeted Therapy: Drugs like bevacizumab that target blood vessel growth in tumours. It can be added to chemotherapy in recurrent or metastatic cervical cancer and has been shown to improve survival.
- Immunotherapy: agents such as pembrolizumab for PD-L1-positive tumours are used in advanced or recurrent cases. These newer treatments are usually offered in specialist centers after a careful assessment of tumour markers (such as PD-L1 expression) and overall health.
- Supportive and palliative care: This is essential to maintain quality of life. Examples include : i. Pain management: essential for quality of life. ii. Nutritional support: To address weight loss from treatment. iii. Psychosocial support: Counselling and groups to cope with emotional impacts. Iv Management of treatment side effects – such as fatigue, bowel and bladder changes, menopausal symptoms or sexual difficulties.
These newer treatments are usually offered in specialist centres after careful assessment of tumour markers (such as PD-L1 expression) and overall health.
Support and Resources
Check out the following links for support and resources on cervical cancer: