What is colorectal cancer?
Colorectal cancer is a disease that arises when the cells lining the colon (large intestine) or rectum undergo abnormal genetic changes (DNA mutations) and begin to grow uncontrollably. These cells live longer than normal, form masses (tumours), and can invade nearby tissues. In advanced stages, the cancer spread to distant organs such as the liver and lungs through a process called metastasis.
There are about 1.9 million new cases and approximately 935000 deaths attributed to colorectal cancer in 2020. The burden of the disease is rising, particularly in low- and middle-income countries where access to screening and early treatment is limited, with more deaths due to late-stage diagnosis.
Why Do People Develop Colorectal Cancer?
Colorectal cancer develops from a combination of genetic and lifestyle-related factors. Researchers have found that a healthy lifestyle may help mitigate the risk of colorectal cancer even in people who are genetically predisposed. Colorectal risk factors include the following:
- Genetics and Family History: Inherited genetic conditions such as Lynch syndrome and Familial Adenomatous Polyposis (FAP) significantly increase the risk of colorectal cancer. People with a strong family history are advised to undergo screening at an earlier age and more frequently.
- Age: The likelihood of developing colorectal cancer increases with age, especially after 50 years.
- Diets: Diets high in red and processed meats, as well as those low in fibre, are associated with an increased risk of colorectal cancer. In contrast, diets rich in fruits, vegetables, and whole grains are protective.
- Obesity and Physical Inactivity: Obesity elevates the risk of colorectal cancer, possibly due to altered levels of the hormone insulin and chronic inflammation in heavier individuals. In particular, increased fat deposition around the abdomen has been identified as an important risk factor.
- Other Medical Conditions: People with inflammatory bowel diseases (e.g., Crohn’s disease and ulcerative colitis) have an increased risk of colorectal cancer. In these conditions, prolonged irritation leads to cellular changes that promote uncontrolled growth, resulting in the formation of cancerous tumours (masses).
How is colorectal cancer diagnosed?
Colorectal cancer can be diagnosed through thee following methods:
- Stool-based tests (screening) such as the faecal occult blood test (FOBT) and faecal immunochemical test (FIT) detect hidden blood in stool, which might serve as a pointer to colorectal cancer.
- Colonoscopy: A flexible tube with a camera is inserted into the rectum to view the colon and take samples.
- Sigmoidoscopy: Similar to colonoscopy but examines only the lower part of the colon.
- Biopsy: a small tissue sample is taken from suspicious areas in the colon or rectum during colonoscopy and sent to the laboratory. The sample is processed and examined under a microscope by specialist doctors (histopathologists) to confirm cancer.
- Imaging techniques such as CT scans or MRI may also be used to assess cancer spread.
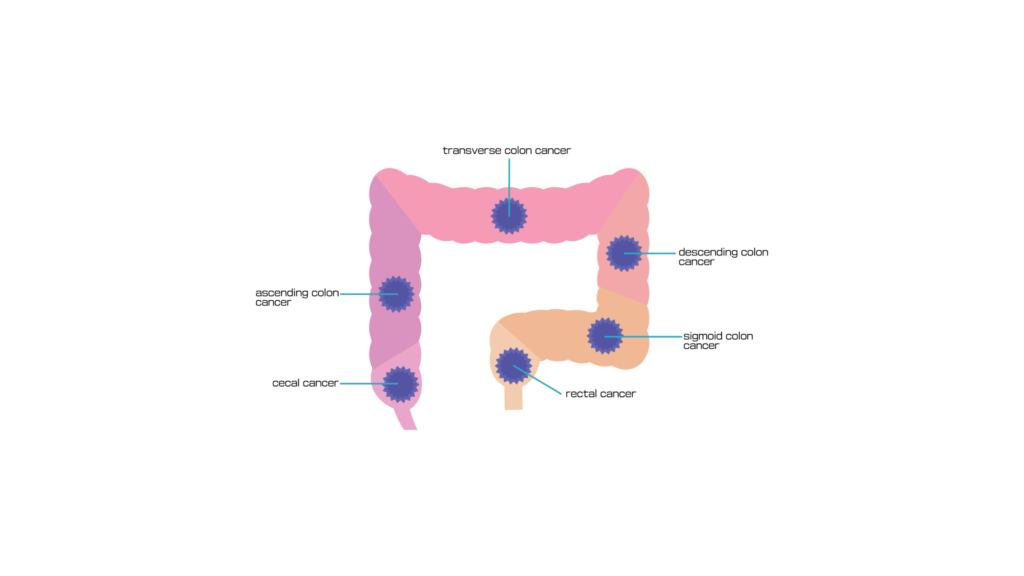
What are the types of colorectal cancer?
Colorectal cancers are classified based on their cellular origin:
1.Adenocarcinoma: The most common type arises from glandular cells that line the colon or rectum. They could be non-invasive or invasive.
Non-invasive (in situ): Cancer cells are limited to the inner lining.
Invasive: Cancer cells infiltrate deeper layers and can spread to lymph nodes or other organs such as the liver or lungs.
2.Carcinoid Tumours: rare, slow-growing tumours originate from hormone-producing cells of the intestines.
3.Gastrointestinal Stromal Tumours (GISTs): They develop from specialised cells in the gut wall.
4.Other tumours: There are other types based on tissue structure (histological appearance), such as lymphomas or sarcomas.
What are the symptoms and signs of colorectal cancer?
You may experience the following symptoms if you have colorectal cancer, depending on the stage of the disease:
- Changes in bowel habits: persistent diarrhoea, constipation, or a feeling that the bowels don’t empty completely.
- Blood in stool: May appear as bright red blood or dark, tarry stool.
- Abdominal discomfort: Cramping, pain, bloating, or gas that doesn’t go away.
- Unexplained weight loss and loss of appetite.
- Fatigue and weakness: Often due to anaemia caused by chronic blood loss.
- Systemic symptoms: In advanced stages, symptoms like jaundice (if spread to the liver) or bone pain appear.
How Can Colorectal Cancer Be Prevented?
- Healthy Weight: Maintaining a healthy weight is important to lower the risk of colorectal cancer. Obesity is linked to increased risk, particularly for colon cancer in men and women.
- Healthy Diet: A diet rich in fruits, vegetables, whole grains, and fibre can lower the risk of colorectal cancer. Reduced intake of red and processed meats has also been associated with decreased risk.
- Physical Exercise: Research has shown that engaging in regular physical activity is associated with a lower risk of colon cancer and improved outcomes for those diagnosed. Exercise may help by regulating body weight, improving digestion, and reducing inflammation.
- Periodic Screening: Colonoscopy or stool-based tests help in early detection by finding polyps before they become cancerous. In many countries, screening is recommended starting at age 45-50, every 10 years for colonoscopy.
- Avoid Smoking and Limit Alcohol: Quitting smoking and moderating alcohol intake can significantly reduce colorec
- Genetic counselling and testing : can help those with a family history of cancers by identifying mutations such as those in Lynch syndrome and Familial Adenomatous Polyposis (FAP). High-risk individuals may consider more frequent screening starting from an earlier age than other people.
What Treatment Options Are Available for Colorectal Cancer?
Colorectal cancer is managed through different methods, including the following
- Surgery: The primary treatment for early-stage disease.
i. Polypectomy: The removal of polyps during colonoscopy.
ii. Colectomy: Removal of part of the colon, often with nearby lymph nodes.
iii. Colostomy: In some cases, an opening is created for faecal elimination when the rectum is removed.
2.Chemotherapy: Use of drugs to destroy cancer cells, given as injections or pills. It may be administered before surgery (neoadjuvant) to shrink tumours or afterwards (adjuvant) to eliminate remaining cells.
3.Radiotherapy: Use of radiation energy to kill cancer cells, often for rectal cancer to shrink tumours before surgery or reduce recurrence risk after surgery.
4.Targeted Therapy: Attacks specific cancer cells without harming normal tissue. Drugs such as bevacizumab (anti-VEGF) and cetuximab (anti-EGFR) target specific cancer pathways.
5. Immunotherapy boosts the immune system to fight cancer and is effective for tumours with specific genetic features, like microsatellite instability (MSI-high).
6.Supportive Treatment:
i. Pain Management: Essential for quality of life in advanced cases.
ii. Nutritional Support: To address weight loss or digestive issues from treatment.
iii. Psychosocial Support: counselling and groups to cope with emotional burdens.
Support and Resources
For more information and support on colorectal cancer, you can visit:
- www.cancerresearchuk.org
- www.macmillan.org.uk
- www.bowelcanceruk.org.uk
- www.cdc.gov/cancer/colorectal
- www.coloncancercoalition.org
- https://fightcolorectalcancer.org/
To read about other forms of cancer, check out:
Breast cancer: https://medhubia.co.uk/breast-cancer-awareness-what-you-need-to-know-about-breast-cancer/
Prostate cancer: https://medhubia.co.uk/prostate-cancer-awareness-understanding-its-risks-symptoms-and-management/
Lung cancer : https://medhubia.co.uk/lung-cancer-awareness-how-much-do-you-know-about-lung-cancer/